The US healthcare market spans hospitals, clinics, insurers, and digital care, making patient experience a key factor in where people seek treatment and whom they trust. Public ratings, higher out-of-pocket costs, and value-based care are pushing providers to focus on service quality as well as outcomes. Consumer surveys reveal how patients perceive access, communication, coordination, and billing across this complex system.
Relying only on internal data often misses why patients switch providers or lose confidence. Experience surveys bring the patient voice into decisions, showing what builds loyalty and where trust weakens. As choices expand and reputations spread quickly, understanding real patient sentiment is essential to sustaining patient relationships.
Why Consumer Experience Surveys Are Essential in Healthcare Market
- Fragmented Patient Journeys Care often moves across hospitals, clinics, insurers, and digital tools, so patients face uneven service at each step. Without structured feedback, organizations struggle to see where journeys break down or which touchpoints damage experience and loyalty.
- Fragile Brand Trust One poor interaction can spread quickly through reviews and social media, shaping public perception. Without continuous feedback, organizations detect issues late, after reputation and referrals have already been affected.
- Value-Based Payment Risk Reimbursement and contracts increasingly link to patient experience scores. Without reliable survey data, organizations cannot track satisfaction or improve metrics, risking penalties, lost incentives, and weaker payer relationships.
- Operational Blind Spots Leaders often rely on internal reports rather than patient voice. Wait times, staff behavior, and process friction persist because real experiences are not captured systematically across locations and service lines.
- Equity And Access Challenges Different patient groups face different barriers in language, affordability, and access. Without segmented surveys, disparities remain unnoticed, exposing organizations to compliance concerns and reputational damage.
Nexdigm’s Healthcare Service Quality Survey Frameworks
Nexdigm approaches healthcare service quality surveys by linking patient feedback directly to care delivery, brand trust, and retention goals. The method brings together structured patient voice capture, benchmarking, and action tracking so organizations can clearly see where experiences succeed or fail across the care journey and respond with targeted improvements.
- Patient Journey Mapping Framework
- Voice of Patient Multichannel Capture
- Experience KPI and Benchmark Model
- Driver Analysis and Loyalty Linkage
- Segmentation and Equity Lens
- Closed Loop Improvement System
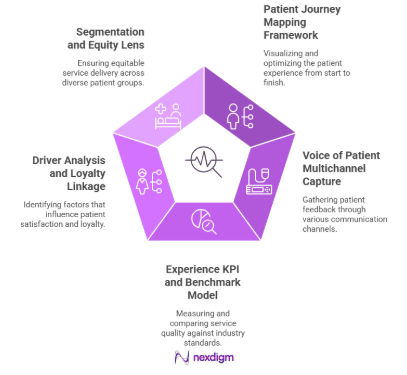
Nexdigm Services for Patient Experience Improvement
- Patient Journey Mapping Framework traces the patient’s real path from first search to follow-up care, highlighting where access, scheduling, wait times, or coordination feel difficult across providers, insurers, and digital channels.
- Voice of Patient Multichannel Capture brings together feedback from post-visit surveys, SMS, email, call-center conversations, and public reviews, creating a single view of patient sentiment across care settings and population groups.
- Experience KPI and Benchmark Model defines clear measures such as satisfaction, trust, clarity of communication, and service reliability, then compares performance across locations, specialties, and market peers.
- Driver Analysis and Loyalty Linkage connects specific experience elements to retention, recommendations, and switching behavior, showing which service factors most influence ongoing patient relationships.
- Segmentation and Equity Lens reviews results by age, condition, coverage type, and community group to surface differences in access, language support, affordability, and perceived fairness of care.
- Closed Loop Improvement System turns insights into action through live dashboards, frontline alerts, root-cause workflows, and ongoing tracking of service improvements across the organization.
Nexdigm’s Case
A US outpatient care network saw falling patient retention despite good clinical results. Nexdigm’s service quality survey identified long appointment waits and confusing billing as main experience gaps. Process fixes and clearer billing communication were introduced. Within two quarters, patient retention rose 18% and patient ratings improved across clinics.
To take the next step, simply visit our Request a Consultation page and share your requirements with us.
Harsh Mittal
+91-8422857704

