In the United States, consumer preference surveys increasingly inform strategy within a value-based care environment, where reimbursement links to quality, experience, and cost efficiency.
Consumer surveys are structured instruments used to collect patient attitudes, expectations, and decision drivers across healthcare services, access, pricing, and outcomes.
Insights on provider choice, digital engagement, care coordination, preventive behaviors, and trust guide benefit design, network configuration, service line prioritization, and patient experience investments.
They help organizations align offerings with patient-perceived value, improve engagement, reduce leakage, and support population health goals while meeting payer performance metrics and competitive differentiation in dynamic US healthcare markets today.
Consumer Preference Surveys in Value-Based Care
- Structured capture of patient-defined value drivers: Consumer surveys systematically identify what patients perceive as quality, convenience, affordability, and trust across the care journey within a value-based care environment.
- Systematic data collection across key preference dimensions: Standardized questionnaires gather patient views on provider choice, access expectations, cost transparency, digital engagement, care coordination, and outcome satisfaction from defined populations.
- Segmentation and gap analysis of consumer insights: Analyzed responses reveal distinct preference segments, unmet needs, and experience gaps linked to utilization patterns, loyalty, and engagement behavior.
- Translation of insights into value-based strategic actions: Organizations apply survey findings to redesign access pathways, optimize provider networks, strengthen care navigation, expand virtual care, and align benefits with perceived value. Support for risk stratification and targeted engagement.
Value Added by Consumer Surveys in Value-Based Care
Healthcare consumer surveys provide sector-wide visibility into patient-defined value, enabling providers and payers to align services with expectations central to value-based care. They inform access redesign, digital channel investment, care coordination models, and benefit structures that improve experience and outcomes.
- Network optimization and access strategy informed by patient provider choice patterns, geographic demand clusters, and appointment availability expectations
- Patient journey and care coordination redesign using experience gaps, transition barriers, and care navigation preferences identified in surveys.
- Digital health adoption and engagement programs aligned to channel preferences, usability drivers, and communication expectations captured from consumers
Nexdigm’s Framework Applies Healthcare Consumer Preference Surveys
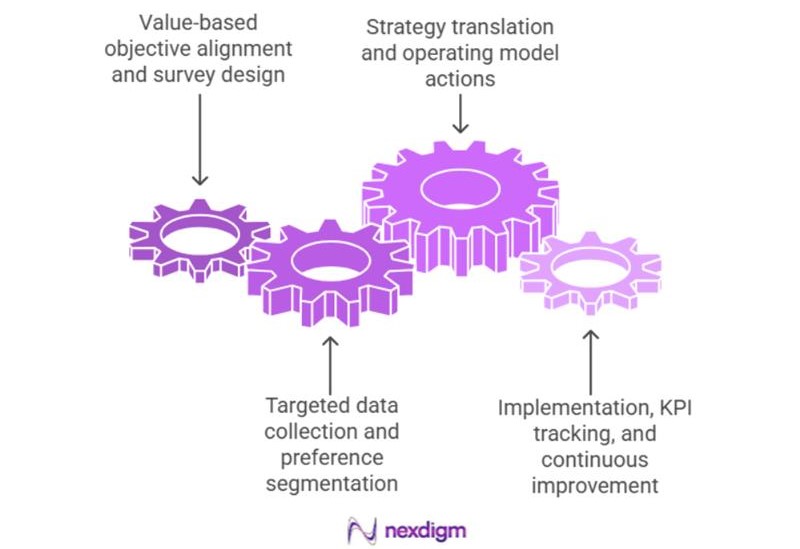
Step 1: Value-based objective alignment and survey design
Nexdigm defines client value-based priorities and designs consumer preference surveys capturing drivers such as access, cost transparency, provider choice, digital engagement, and care coordination mapped to performance metrics.
Step 2: Targeted data collection and preference segmentation
The firm deploys surveys across representative patient cohorts and applies analytics to identify preference segments, unmet needs, and experience gaps linked to utilization and adherence behavior.
Step 3: Strategy translation and operating model actions
Insights are converted into initiatives including access pathway redesign, network optimization, digital front door enhancement, care navigation strengthening, and benefit alignment with consumer-defined value.
Step 4: Implementation, KPI tracking, and continuous improvement
Nexdigm supports execution, establishes value-based KPI dashboards on experience and utilization, and conducts repeat measurement cycles to refine strategy and sustain contract performance.
Nexdigms’ case:
Nexdigm surveyed attributed patients for a US health system in value-based contracts, identifying access gaps and leakage drivers. Extended hours, referral navigation, and digital scheduling improved experience scores 12%, preventive screening 18 percent, and reduced out-of-network leakage 9 percent within two years.
To take the next step, simply visit our Request a Consultation page and share your requirements with us.
Harsh Mittal
+91-8422857704

