The United States healthcare economy exceeds USD 4.5 trillion in annual spending, spanning hospitals, insurers, and outpatient services. Patient experience increasingly determines provider choice and lifetime value across competitive regional markets. Quality surveys convert perceptions into measurable retention drivers insights.
Without structured consumer surveys, providers misread expectations and lose patients to higher rated competitors quickly.
- Operational blind spots persist, eroding loyalty, referrals, and reimbursement performance over time and margins decline.
- Service gaps remain unidentified across care journey touchpoints leading attrition.
- Staff training priorities misaligned with patient experience drivers and complaints.
- Investment decisions ignore satisfaction data, weakening retention economics and growth.
Business Strategy Areas Improved by Consumer Survey Insights
Consumer survey insights translate patient voices into actionable priorities across clinical, operational, and commercial healthcare strategy domains supporting evidence based decisions enterprise. They quantify satisfaction drivers, switching triggers, and loyalty barriers, enabling targeted improvements that measurably strengthen retention and lifetime value across care settings like:
-
Positioning
Clarifies brand promise against local competitors using patient perceptions, differentiators, and trust factors to refine messaging, service mix, and market targeting decisions for growth focus.
-
Operations
Identifies process bottlenecks across scheduling, wait times, discharge, and billing interactions, prioritizing fixes that reduce friction, complaints, and abandonment across care pathways for efficiency gains.
-
Experience
Maps emotional highs and lows along journeys, guiding service design, staff behaviors, environment standards, and communication tone to consistently exceed expectations for loyalty and advocacy.
-
Pricing
Reveals willingness to pay, perceived fairness, and value tradeoffs across services, informing pricing architecture, package design, and financial counseling approaches that support access and margin.
-
Communications
Determines preferred channels, content clarity needs, and information gaps pre and post care, enabling personalized outreach, reminders, education, and reputation management to increase engagement rates.
-
Retention
Segments patients by loyalty risk and drivers, supporting targeted interventions, recovery protocols, membership programs, and followup cadence that improves continuity of care and term retention.
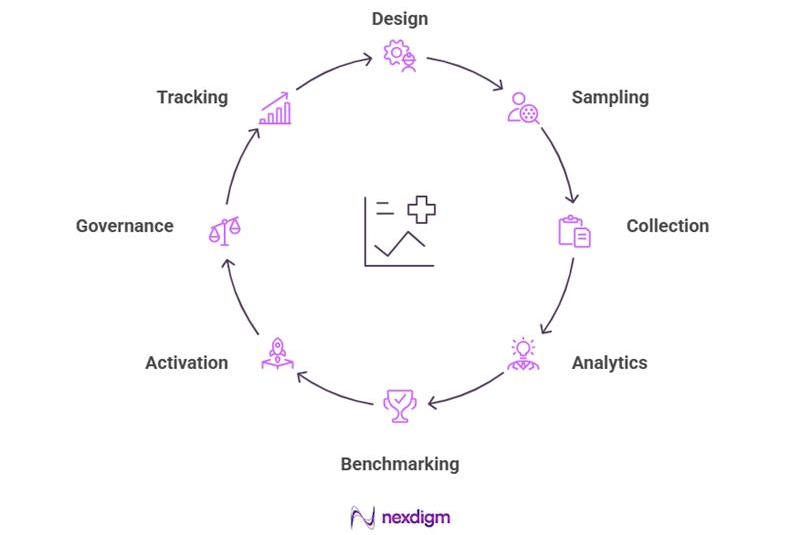
Nexdigm’s Tools and Offerings for Healthcare Consumer Surveys
-
Design
Co creates consumer survey frameworks aligned to service lines, patient journeys, and regulatory requirements, ensuring measurable constructs, benchmarking compatibility, and actionable output across provider settings.
-
Sampling
Builds statistically valid samples across demographics, payer types, and visit categories, reducing bias and enabling reliable comparisons between facilities and specialties over time periods.
-
Collection
Deploys multichannel data capture including SMS, email, web, and kiosk, maximizing response rates while preserving privacy, consent, and accessibility standards for diverse patient groups.
-
Analytics
Applies driver analysis, text mining, and sentiment scoring to isolate satisfaction determinants, root causes, and improvement priorities at granular service levels with clear dashboards.
-
Benchmarking
Benchmarks performance against national surveys and peer providers, contextualizing scores and identifying realistic targets across specialties, regions, and care settings for continuous quality improvement.
-
Activation
Translates insights into prioritized action roadmaps, training modules, and SOP updates, embedding patient experience metrics into management cadence and incentives across clinical and support.
-
Governance
Establishes governance for data ownership, reporting cycles, and escalation, ensuring accountability, compliance with health information regulations, and sustained survey programs enterprise wide oversight mechanisms.
-
Tracking
Implements continuous tracking with dashboards and alerts, measuring intervention impact, retention changes, and ROI, enabling iterative improvement and executive visibility across service lines regularly.
Nexdigm Case
A regional hospital network was losing 18 percent of patients each year and had low experience scores across locations. Nexdigm conducted a structured patient survey across 12 hospitals and clinics, reaching a 32 percent response rate. Results showed problems in appointment wait times, unclear discharge instructions, and confusing bills. The network simplified scheduling, standardized discharge communication, and redesigned billing statements. Within one year, patient loss fell to 11 percent and satisfaction scores rose by 14 points, improving retention and patient loyalty across the system.
To take the next step, simply visit our Request a Consultation page and share your requirements with us.
Harsh Mittal
+91-8422857704

